  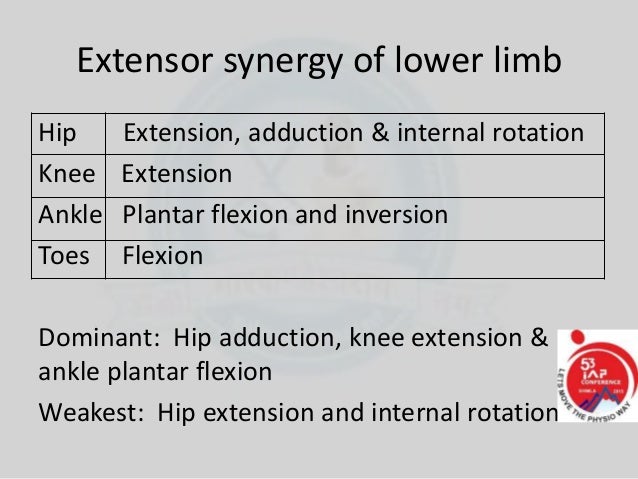 
The human upper extremity is capable of performing a myriad of functional tasks due to its biomechanical structure and its abundant motor and sensory neural innervation. Increased cocontraction of the hand muscles due to increased neural couplings between the distal and proximal muscles appears to be the underlying mechanism. Our results showed significant proximal-to-distal interactions between finger extension and elbow extension/shoulder abduction of stroke survivors exist during their functional movements. Proximal kinematics of stroke survivors was also affected by the finger extension, but the cocontraction of their proximal muscles did not significantly increase, suggesting the changes in the proximal kinematics were made voluntarily. Cocontraction of the extrinsic hand muscles of stroke survivors significantly increased at these locations, where an increase in the intermuscular coherence between distal and proximal muscles was observed. Distal kinematics of stroke survivors, particularly hand opening, were significantly affected by the proximal kinematics, as the hand aperture decreased and the duration of hand opening increased at the locations that requires shoulder abduction and elbow extension. Fourteen subjects, including nine chronic stroke survivors and five neurologically-intact subjects participated in an experiment involving transport and release of cylindrical objects between locations requiring distinct proximal kinematics. In this pilot study, we elucidated proximal–distal interactions and their functional impact on stroke survivors by quantitatively delineating how hand and arm movements affect each other across different phases of functional task performance, and how these interactions are influenced by stroke. 6Department of Mechanical Engineering, Korean Advanced Institute of Science and Technology, Daejeon, South Koreaĭespite its importance, abnormal interactions between the proximal and distal upper extremity muscles of stroke survivors and their impact on functional task performance has not been well described, due in part to the complexity of upper extremity tasks.5Department of Physical Medicine and Rehabilitation, Northwestern University, Chicago, IL, United States.4UNC/NC State Joint Department of Biomedical Engineering, North Carolina State University, Raleigh, NC, United States.3Department of Internal Medicine, Yale University School of Medicine, New Haven, CT, United States.2Center for Applied Biomechanics and Rehabilitation Research, National Rehabilitation Hospital, Washington, DC, United States.1Department of Biomedical Engineering, Catholic University of America, Washington, DC, United States.Abnormal flexor synergy in both hip and knee joints (score 1 or 2) on the Fugl-Meyer Assessment Lower Extremity section II: Volitional movement within synergies (Fugl-Meyer et al.Thanh Phan 1 Hien Nguyen 2 Billy C.Able to walk with or without an assistive device for 7 m independently.Time post-stroke between 6 months and 3 years.Heart rate (HR) will be monitored continuously using a fingertip pulse monitor to ensure the maximum training HR is no more than 75% of the subject's HR Reserve. With feet strapped to the pedals, the participant will be asked to activate the hip, knee, and ankle flexors simultaneously when the pedal is moving up and then relax. The bike pedals are moving backward at a preset speed regardless of user effort. 
Their lower limb muscle function and walking performance will be assessed at baseline (2 to 3 times within the 2 weeks prior to starting the training), at the end of training, and 4 weeks later.Įach subject will perform biking exercises under supervision, 2-3 times per week for 4 weeks (30 minutes each). Ten participants with chronic stroke will be recruited. Therefore, it is the intent of this exploratory study to find out whether an exercise training program focusing on lower limb flexors can improve lower limb motor function late after stroke. Many previous studies have focused on strengthening the lower limb muscles that support the body in standing and walking (the so-called anti-gravity extensor muscles) but the training targeting the lower limb flexors has rarely been emphasized in stroke rehabilitation. It is known that the muscles that flex the hip, knee, and ankle joints are responsible for bringing the leg up and forward during walking and for a successful recovery from a slip or trip. Why Should I Register and Submit Results?. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
